C3 glomerulopathy (C3G) and primary (idiopathic) immune complex–mediated membranoproliferative glomerulonephritis (IC-MPGN) are two different, extremely rare kidney diseases that share a common issue: excessive activation of the C3 protein in the immune system. Normally, C3 helps protect the body from infections, but when it becomes overactive, it can damage the kidneys. Deposition of C3 in the kidneys leads to inflammation and damage of the glomeruli—the tiny filters in the kidneys responsible for removing waste and excess fluid.
Despite being distinct conditions, C3G and primary IC-MPGN have overlapping symptoms, including:
- Proteinuria (high levels of protein in the urine)
- Reduced kidney function
- C3 deposits in the kidney
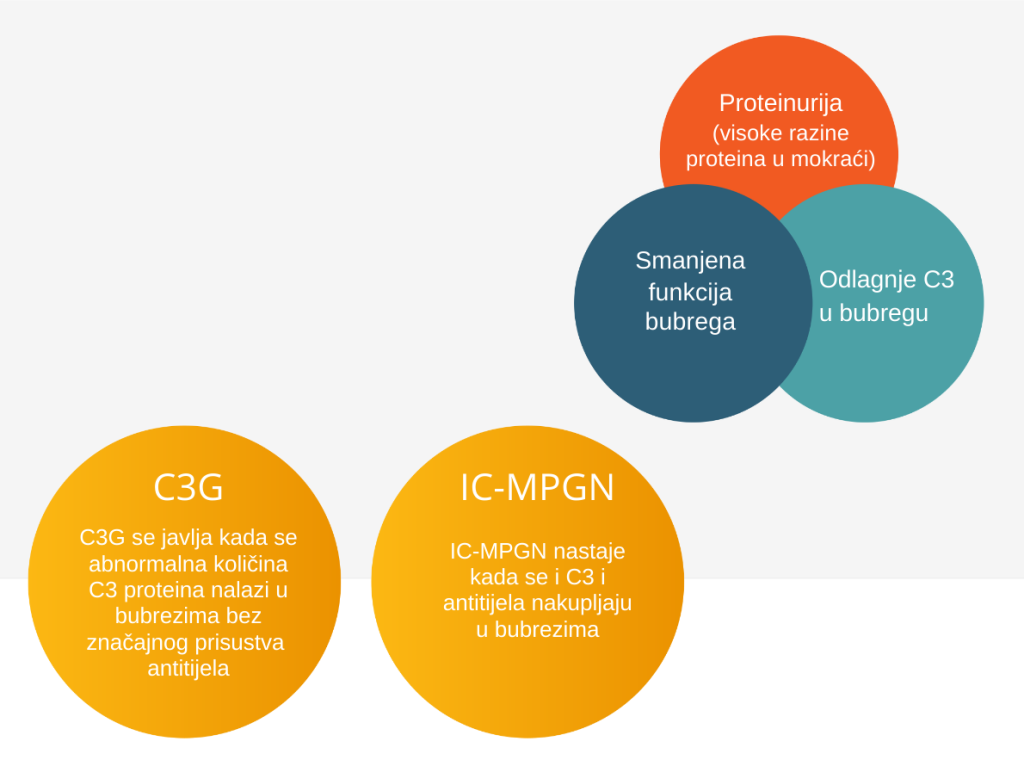
While C3G and primary IC-MPGN are similar, they are caused by different underlying processes in the body. Finding these differences in a biopsy helps your doctor provide an accurate diagnosis and choose the best care plan.
These conditions can affect anyone, but they are most commonly diagnosed in childhood or early adulthood. They affect males and females equally, and in most cases, there is no clear reason why they develop. However, some people may have a higher risk if they have:
- A family history of kidney disease
- Certain genetic factors that affect how their immune system and kidneys work
While certain factors may contribute to disease development, these are not things you could have controlled or prevented.
Signs and symptoms of C3G and primary IC-MPGN
C3G and primary IC-MPGN disrupt the kidney’s ability to f ilter blood effectively, leading to similar signs and symptoms:
- Proteinuria - Excess protein in the urine, often causing foamy or frothy urine.
- Swelling (oedema) - Fluid retention, particularly in the legs, ankles, hands, and around the eyes.
- Hypertension (high blood pressure) - A common symptom that can worsen kidney damage over time.
- Haematuria (blood in the urine) - Urine may appear pink, red, or brown, or microscopic blood may be detected during testing.
- Fatigue and weakness - Caused by the build-up of waste products in the blood and sometimes worsened by anaemia
- Decreased kidney function - Often identified through blood tests, such as elevated creatinine levels, and can progress to kidney failure in severe cases.
Symptoms can vary depending on the stage of the disease and any underlying conditions that might be contributing to the kidney damage.
C3G and primary IC-MPGN diagnosis
People showing signs and symptoms of kidney dysfunction may be asked to go through a range of diagnostic procedures:
- Medical history and physical examination to assess symptoms, family history, and underlying conditions.
- Urine and blood tests to test for proteinuria and haematuria.
- Kidney biopsy to assess structural changes in the kidney and complement or immune complex deposits.
- Genetic and complement tests to identify abnormalities in the complement system that can contribute to kidney damage.
- For primary IC-MPGN, additional tests are conducted to rule out secondary causes and underlying conditions.
This may feel like a lot of tests, but they are essential for getting a clear and accurate diagnosis. Some patients may experience anxiety about kidney biopsy, which is a common response to invasive diagnostic procedures, but it is the only reliable way to confirm C3G or primary IC-MPGN. Having the accurate diagnosis ensures the right care and the individualised treatment plan.
Both C3G and primary IC-MPGN are chronic progressive diseases and, if left untreated, may result in irreversible damage.
The early diagnosis allows for timely treatment, which can allow for timely and individualised care plan to be put in place.
To learn more about C3G and primary IC-MPGN, here are other resources available for you:
Literature
- Bomback AS, Charu V, Fakhouri F. Challenges in the Diagnosis and Management of Immune Complex-Mediated Membranoproliferative Glomerulonephritis and Complement 3 Glomerulopathy. Kid ney Int Rep 2024; 10(1):17-28. doi: 10.1016/j.ekir.2024.09.017. Available from: https://www.kireports.org/article/S2468-0249(24)01945-4/fulltext
- Orphanet (2024). C3 glomerulopathy. Dostupno na: https://www.orpha.net/en/disease/detail/329918
- Caravaca-Fontán, F., Lucientes, L., Cavero, T., and Praga, M. (2020). Update on C3 Glomerulopathy: A Complement-Mediated Disease, Nephron, 144(6), pp. 272–280.
- Noris, M., Donadelli, R. & Remuzzi, G. (2019). Autoimmune abnormalities of the alternative complement pathway in membranoproliferative glomerulonephritis and C3 glomerulopathy. Pediatr Nephrol, 34, pp. 1311–1323 (2019).
- Caravaca-Fontán, F., Toledo-Rojas, R., Huerta, A. et al. (2025). Comparative analysis of proteinuria and longitudinal outcomes in immune complex membranoproliferative glomerulonephritis and C3 glomerulopathy. Kidney International Reports. In press: www.sciencedirect.com/science/article/pii/S246802492500049X
- ERKNet – C3G and IC-MPGN (2025). Dostupno na: https://www.erknet.org/patients/your-kidney-disease/c3g-ic-mpgn/disease-information
